Conditions We Treat
Heel Pain - (Plantar Fasciitis, Heel Spurs, Nerve Entrapment)
Heel pain is one of the most common foot conditions that we see at Southern Tas Podiatry Clinic. We aim to have your pain reduced when you walk out of the clinic and work with you to design a treatment plan that you can do at home. Depending on the severity of your heel pain, treatment usually requires 1 to 4 visits for the best outcomes. The terms plantar fasciitis and heel spur is used interchangeably for heel type pain.
 | Signs and Symptoms of Heel Pain
|
Ankle Pain and Sprains
What Makes an Ankle Hurt?
The ankle is a joint where the bones of the feet and legs meet. The up and down motion of the foot is controlled with this joint. The joint itself as well as the very bottom portion of the leg and the flat part of the upper foot are all considered part of the ankle area. Inflammation or injury to the cartilage, muscles, tendons, ligaments, and bones inside the ankle can all cause the ankle to hurt. Common causes of ankle pain usually include:
|
|
 |
|
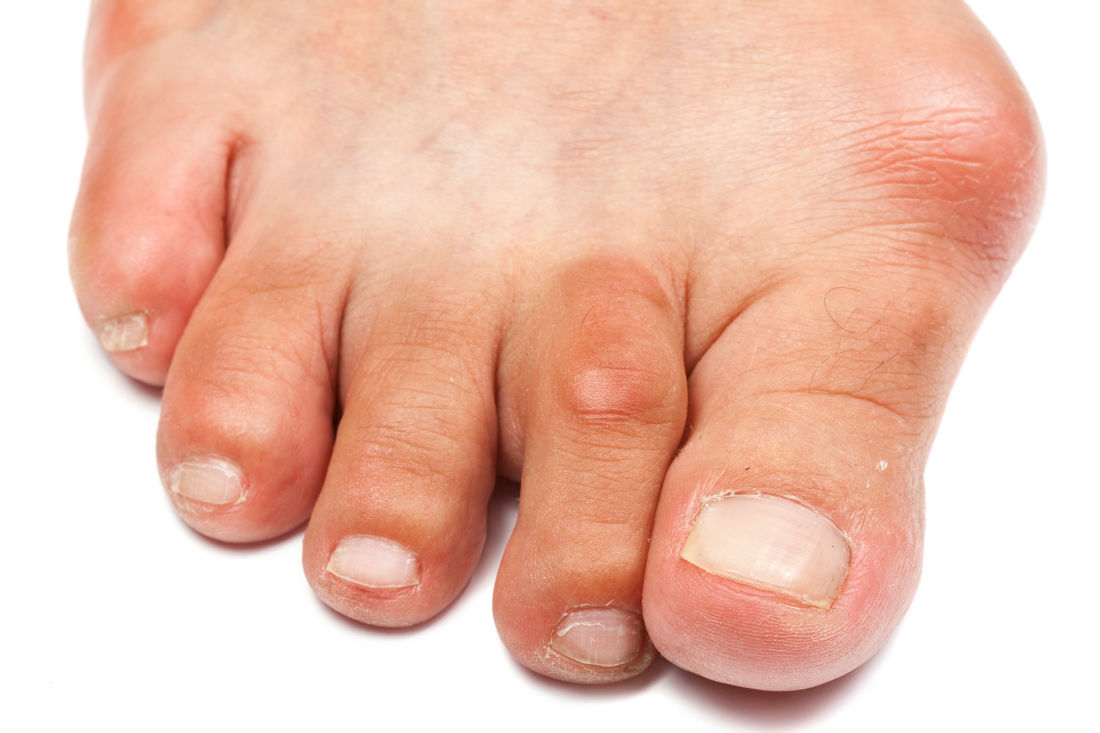
Bunions (Hallux Abducto Valgus)
Bunions are a common painful condition which affect our feet. Women are more prone to this problem than men. A bunion is a bony lump usually over the joint between the big toe and the rest of the foot. This creates a pressure point when shoes are worn, producing the painful, red swelling lump known as a bunion.
 |
|
Achilles Tendinopathy
Achilles Teninopathy (Tendonosis/Tendonitis) is micro damage to the Achilles Tendon. The Achilles Tendon is the strongest tendon in the body, connecting the calf muscles to the heel bone behind the ankle joint.
 |
|
Shin Splints - Medial Tibial Stress Syndrome
Shin splints are a common lower extremity complaint, especially among runners and athletes. Typically, the pain is associated with overuse of the muscles and affects the front lower leg.
Pain usually develops gradually and may begin as a dull ache. Small bumps and tender areas may develop adjacent to the shin bone. The pain can become more intense if not addressed, and shin splints should not be left untreated because of an increased risk of developing stress fractures.
 |
|
What Causes Foot Pain?
Feet carry the weight of a person and are put under great strain each and every day. When pain in the feet becomes a chronic concern many conditions or issues can be to blame such as:
| • Gout and arthritis • Bunions and hammer toes • Tendonitis • Plantar fasciitis • Flatfeet and fallen arches • Calluses and corns | • Turf Toe • Heel spurs • Stress fractures • Ingrown toenails • Nerve Damage • Broken bones and toes |
 |
|
Biomechanical Gait Analysis
If you can understand how you move – and the impact this can have on your body and overall health – then you are well placed to resolve a range of health issues early on.
 |
|
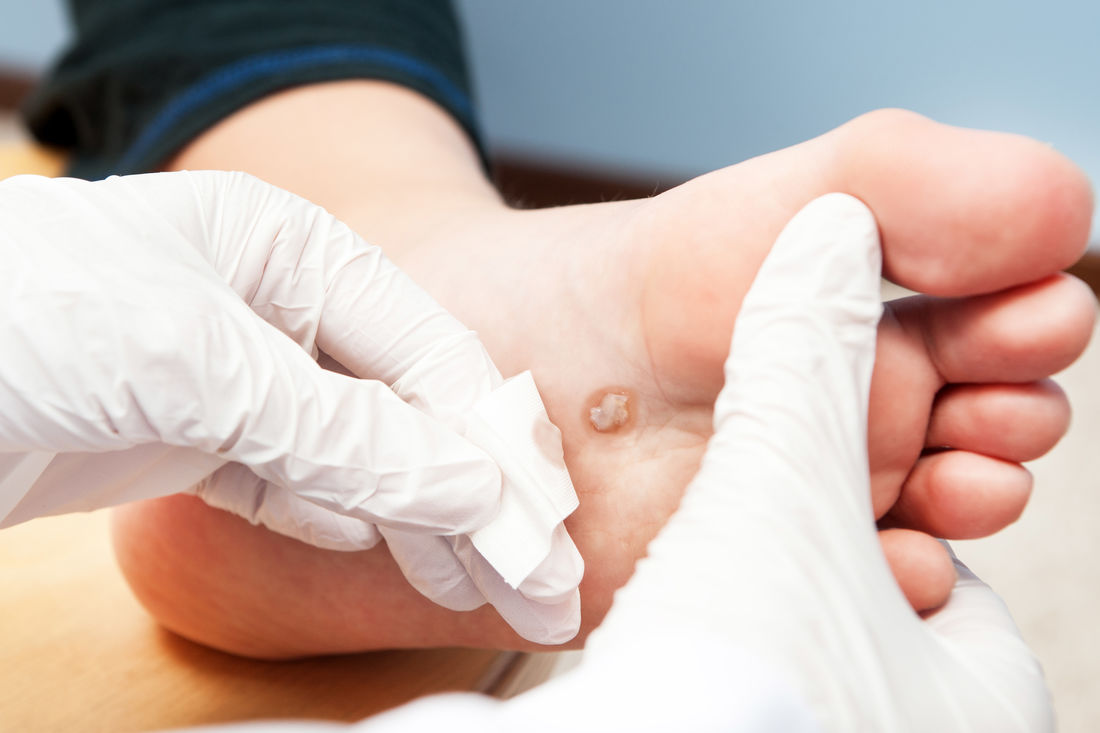
Plantar Warts
All types of people can be affected by plantar warts. At Southern Tas Podiatry Clinic we treat plantar warts.
 |
|
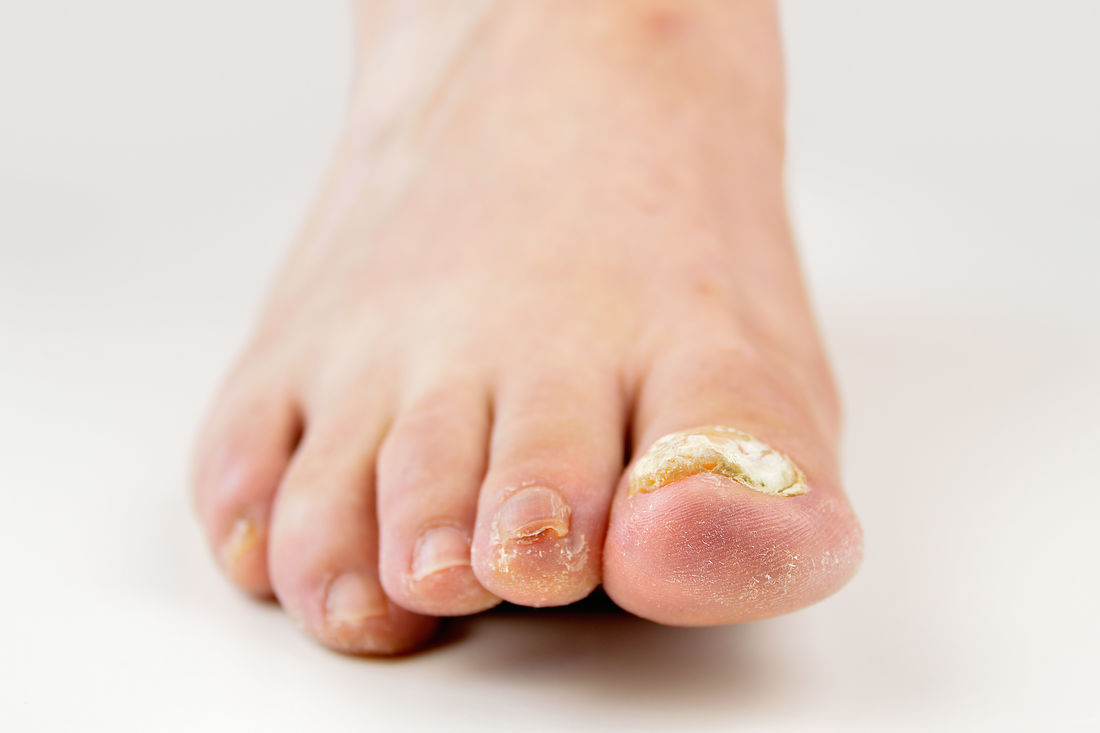
Fungal and Nail Infections
Read on to see how to avoid these types of infections, and what to do if you have an infection on your feet or toenails.
Nail fungus is often caused by something called ‘dermatophytes’, which are fungi found growing on skin, hair, nails and other bodily surfaces. When dermatophytes get underneath your nail, it causes A yellow brownish or white discolouration and the nail can become thick and crumbly.
You can live with a fungal toenail, though sometimes if left untreated the skin underneath your nail can become inflamed and/or painful. If you are comcerned or having pain from fungal toenails please contact us for treatment and advice. .
 |
|
Skin & Nail Treatment
Toenail Problems
Your podiatrist will check the condition of your toenails and help you understand the health implications of their appearance, as well as providing a range of treatments for any toenail problems.
Any sudden changes in colour or shape of the toenail, signs of infection, development of a freckle under the nail, or unexplained pain should be discussed with your podiatrist immediately. Your podiatrist can diagnose the problem and arrange appropriate treatment.
Corns & Callus (Hard Skin)
Calluses and corns are generally signs of underlying problems and, in some cases, early warning signals of more complex foot disorders.
Your podiatrist will not only recommend ways to relieve pain and get rid of the corn or callus, but can also help with isolating the cause and preventing the problem from recurring.
 |
|
